In an effort to reduce healthcare costs for Americans, the Biden administration is negotiating the first-ever medicine prices for Medicare with manufacturers of the blood thinner Eliquis, the diabetic treatment Jardiance, and eight other pharmaceuticals.
The ten medications for which pricing would be discussed directly with the manufacturer were listed by the administration on Tuesday. Although the action is anticipated to lower costs for many patients, drug manufacturers are suing it and Republican politicians have harshly criticised it, so it will be years before consumers see any savings.
The initiative is the focus of President Joe Biden’s reelection campaign as the Democrat looks to convince voters that he deserves another term for the work he’s doing to reduce costs for them while the nation battles inflation. But much of Biden’s most significant policy changes need time to implement, much like the drug negotiations, so his job is to convince the public to wait.
“For many Americans, the cost of one drug is the difference between life and death, dignity and dependence, hope and fear,” Biden said in a statement. “That is why we will continue the fight to lower healthcare costs — and we will not stop until we finish the job.”
Later on Tuesday, Biden intends to speak about health care prices from the White House. Kamala Harris, vice president, will be present with him.
According to the Centres for Medicare and Medicaid Services, or CMS, the pharmaceuticals on the list that was released on Tuesday were responsible for more than $50 billion in Medicare prescription drug costs between June 1, 2022, and May 31.
The government organisation also reported that Medicare patients who used the medications last year had out-of-pocket expenses of $3.4 billion.
Eliquis and Jardiance
The list included the diabetes medications Jardiance from Eli Lilly and Company, Boehringer Ingelheim, and Januvia from Merck. Enbrel, a medication used to treat autoimmune diseases, and Entresto, a medication used to treat heart failure, were also included.
According to AARP research, Medicare spent roughly $10 billion in 2020 on Eliquis. The medication from Pfizer and Bristol-Myers Squibb addresses blood clots in the legs and lungs and lowers stroke risk in adults with atrial fibrillation, an abnormal heartbeat.
According to senior administration officials, some of the 10 medications chosen for negotiation are among the most expensive for the Medicare programme. 8.2 million Medicare Part D beneficiaries, according to them, use them.
Also Read: Johnny Manziel’s father faked a heart attack to help Cleveland Brown’s quarterback skip drug test
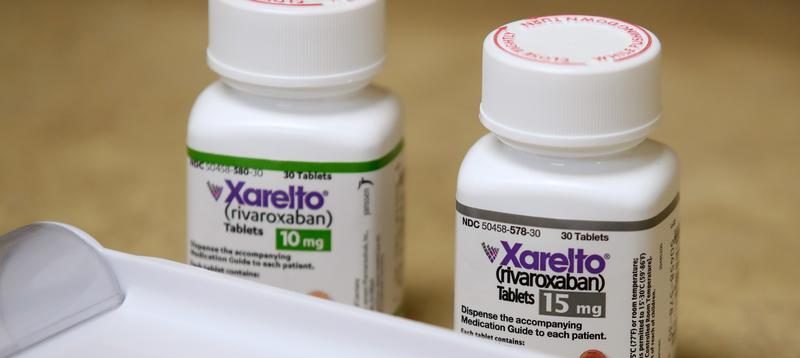
The diabetic and heart failure medication Farxiga from AstraZeneca is also included, as are three medications from Johnson & Johnson: the blood thinner Xarelto, the blood cancer medication Imbruvica, and its top selling, Stelara, an intravenous therapy for psoriasis and other inflammatory conditions.
Numerous variations of Novo Nordisk’s fast-acting insulin Fiasp, which is administered around meals, are also included on the list.
The Medicare patient out-of-pocket expense for insulin is already limited to $35 per month under the Inflation Reduction Act. Tuesday, a representative of the administration stated that although the highest ceiling will remain in place, those expenses might vary further.
The Inflation Reduction Act, which Biden signed last year, has advanced with this news.
The administration wants to negotiate the pharmaceuticals on the list that was made public on Tuesday for the lowest possible fair price. That would be helpful for some individuals who have insurance but still must pay hefty expenses for prescriptions with high deductibles.
According to research by the Commonwealth Fund, a think tank that investigates health care issues, almost 9% of Medicare recipients aged 65 and over reported in 2021 that they skipped a medication dose or did not fill a prescription because of the expense.
Also Read: Who is Dairo Antonio Úsuga David? Colombian drug lord jailed for 45 years by US court
Right now, pharmacy benefit managers that handle Medicare prescription coverage bargain for discounts on drug costs. These rebates can occasionally lower the premiums that customers must pay for insurance. However, they might not affect how much money a patient pays at the pharmacy counter.
Negotiation Plans
The new drug price negotiations aim “to basically make drugs more affordable while also still allowing for profits to be made,” said Gretchen Jacobson, who researches Medicare issues at Commonwealth.
Drug companies that refuse to be a part of the new negotiation process will be heavily taxed.
The government will present its initial proposal for a maximum just price by February 2024, after which drug manufacturers will have opportunity to respond.
Any agreed-upon prices won’t go into effect until 2026.
For 2027 and 2028, CMS intends to add 15 more medications to its negotiation list. After that, it intends to add up to 20 more for each succeeding year.